Gentle readers,
It is flu shot season. And do-the-physicals-on-your-Medicare patients-before-they-go-somewhere-else-and-another-office-bills-the-physical season. And I am seeing a lot of the same question from both my billing service providers, and from you, my gentle readers.
Specifically, you billed/coded the flu shots and physicals the way I taught you and they are still getting denied! What gives?
And here is your unfortunate answer.
Medicare will pay a flu shot once every 365 days. They will pay a physical once every 365 days. They will pay a pap once every 730 days for a woman at normal risk and once every 365 days for a woman at high risk. They will pay the pneumo vaccine once every 365 days.
That means that if a patient came in on Feb 17th 2016 to get their flu shot last year and then came in this year on Jan 25th and got another flu shot, you will not get paid. Even if you bill with ICD10 Z23. Even if you bill with the Q-code for the vaccine. Medicare does not care that it is a different flu season. They do not care that your patient will be visiting their newborn grandson in a couple weeks and they need to be up to date on their immunizations. They do not care that your patient is going for a month long cruise in the caribbean and this is the last date they have available until they get back and they would prefer to get it done before they are rubbing elbows with a bunch of strangers who may have the flu.
Medicare does not care.
And they really mean 365 days. Not 364. So, when a patient needs a preventive service, please try and train your doctors and your office staff to check the date the patient received their last preventive service. The Medicare site also has a tab under the eligibility lookup section to check and see when the patient is next eligible for a preventive service. Here is a screenshot of the page and what it looks like:
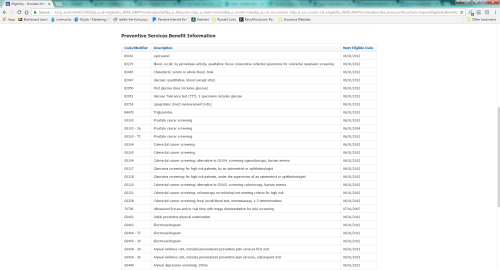
As you can see, the date the patient is going to be eligible for any specific service is indicated on the right. Flu and Prevnar are not included in this list, so you will need to rely on your records to track those.
Below is the link to a good website for more information on the Medicare policies for preventive services.
Keep emailing your questions and I’ll keep giving you answers.
